|
8/2/2023 0 Comments Pellucid eye 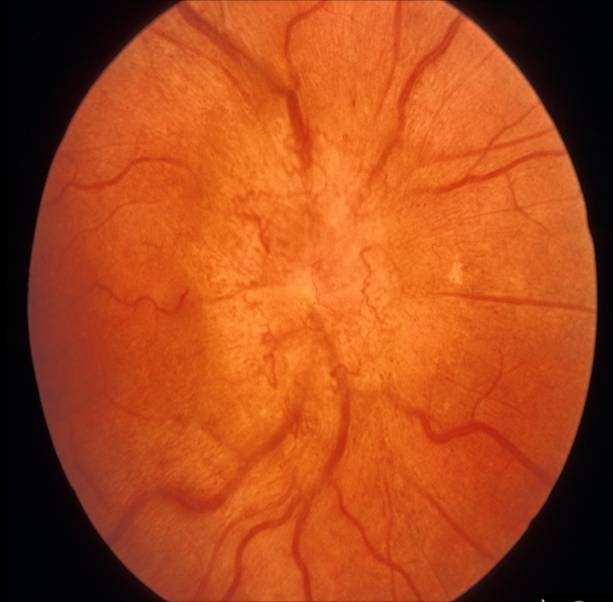 
This case illustrates the clinical efficacy of amniotic membrane grafting as an effective alternative in the management of spontaneous corneal perforation resulted from pellucid marginal degeneration. The corneal integrity was restored with resolution of the corneal edema and the visual acuity improved from 20/400 before surgery to 20/40 three months later. There was no aqueous leakage on the first post- operative day. Amniotic membrane grafting using both a surgical graft and a bandage patch was thus performed in the operating room the following day. The initial management with cyanoacrylate tissue adhesive and bandage contact lens did not preclude aqueous leakage the next day. Received 8 July 2015 accepted 27 November 2015 published 30 November 2015Ī 47-year-old woman with a history of pellucid marginal degeneration was referred for management of hydrops and peripheral perforation of the right cornea. This work is licensed under the Creative Commons Attribution International License (CC BY). During your examination, you will learn about your candidacy for scleral lenses, including an estimate of out-of-pocket costs.1Department of Ophthalmology, Keck School of Medicine of the University of Southern California, Los Angeles, CA, USAĢDepartment of Ophthalmology, The Wilmer Eye Institute, The John Hopkins University, Baltimore, Maryland, USAĬopyright © 2015 by authors and Scientific Research Publishing Inc. To learn more about your keratoconus, call ReVision Optometry today to schedule your examination at 619.299.6064 or request an appointment online. These days, scleral contact lenses are a common and effective treatment for keratoconus, including if your eye doctor diagnosed PMD. The treatment to restore vision is the same if you have PMD or classic keratoconus: specialty contact lenses with a rigid surface are the gold standard for visual rehabilitation. If your doctor told you that you have PMD, you likely get decent vision with updated eyeglasses and received diagnosis later in life compared to others with keratoconus. PMD is the same thing as keratoconus, just a subclass of it. The fact that some patients have a PMD-type topography in one eye and a more classic keratoconus topography in their other eye, also supports that these are the same disease entity. 
In other words, most patients with PMD likely had onset of their corneal distortion in the adolescent years despite diagnosis coming much later due to mild symptoms. Since many patients with PMD achieve good vision with eyeglasses with the bulk of the corneal distortion decentered downward out of the line of sight, PMD would often get diagnosed later because vision symptoms often are more subtle. Many eye doctors and patients incorrectly assumed that the time of diagnosis was also the time of onset. But in fact, PMD is often diagnosed later because it tends to impact vision less. Second, PMD supposedly had a later onset in life. Reprocessing an axial topography to tangential view generally uncovers a classic keratoconus pattern for most alleged cases of PMD (Figure 2). A topography can be viewed as an “axial map” which smooths out data points, or as a “tangential” map which provides a more point-to-point assessment of light bending power. First, the classic “crab-claw” or “butterfly” topography pattern attributed to PMD (Figure 1) was just due to the way the topographical map was viewed. Two factors previously confused eye doctors into believing that PMD and keratoconus were separate eye conditions. Same topography as Figure 1 but under a tangential view. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
